Due to the COVID pandemic, vaccinations and vaccine hesitancy are on everyone’s lips all over the world. Vaccination is recognized as one of the most groundbreaking medical inventions. However, the changing perception of its safety and effectiveness has led to a growing number of people becoming more hesitant towards vaccines. Increase in outbreaks and decrease in vaccine coverage rates is caused by a phenomenon called vaccine hesitancy. Vaccine hesitancy means reluctance or refusal to vaccinate despite the availability of vaccines. According to World Health Organization, vaccine hesitancy is one of the ten global health threats. (Dube et al. 2013; WHO 2019.)
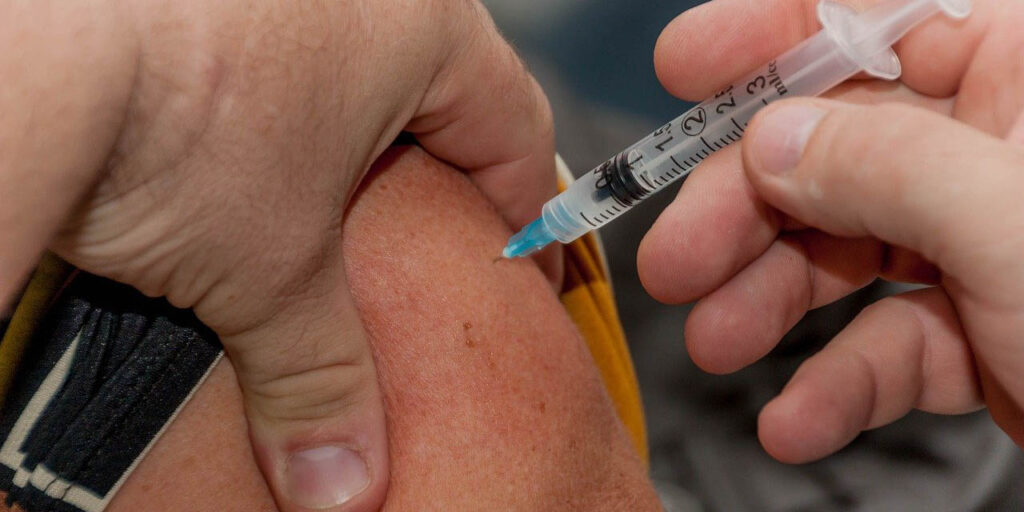
Reasons behind vaccine hesitancy
The causes behind vaccine hesitancy are complex. According to the literature review of Korkawin & Vehmas (2021), many personal and cultural factors dictate vaccination decision-making. Norms, values, behaviors, and experiences affect vaccine views and beliefs, and influence anti-vaccine attitudes. Vaccine hesitancy determinants are also associated with perception of health, politics, religion, and risks. (Succi 2018; Olson et al. 2020.)
Nowadays, it is difficult for people to distinguish evidence-based knowledge from misinformation. Many non-official websites seem trustworthy, but in reality, are misleading and manipulative. Anti-vaccine culture thrives in people’s dependance on the internet as a source of information to spread misconceptions. Media-consumerism has caused doubts, concerns, and mistrust towards vaccines. (Poland et al. 2009; Dube et al. 2013.) The internet and social media platforms are effective platforms for spreading mis- and disinformation. This phenomenon has been well seen during the recent COVID pandemic.
Tackling vaccine hesitancy
Health care providers play an important role in the implementation of national vaccination programmes and in maintaining vaccine coverage. Patients have the right to receive reliable and up-to-date information on vaccinations in an open, non-judgmental environment. (Paterson et al. 2016; Di Pietro et al. 2017.)
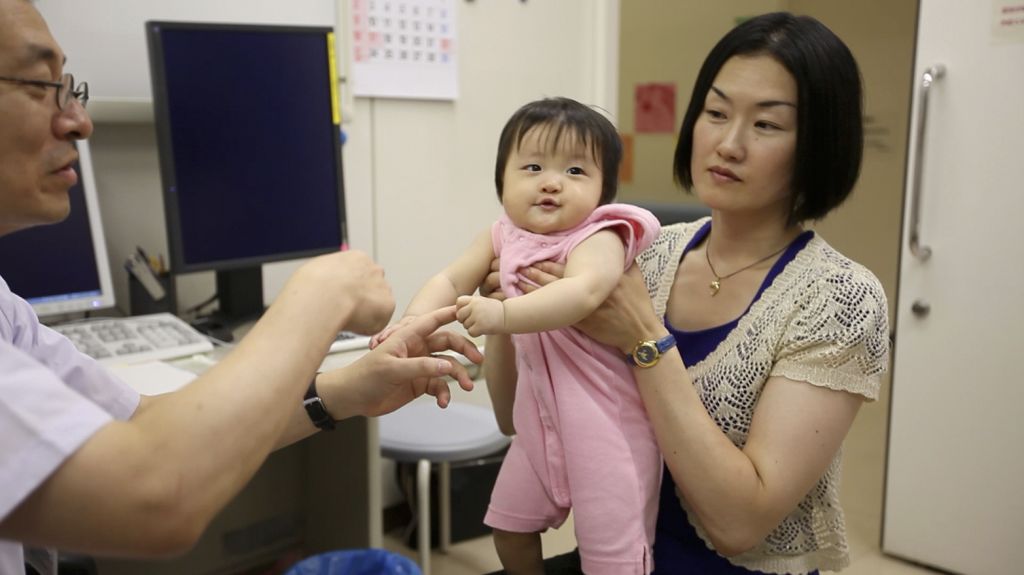
Health care providers should be able to guide clients on vaccination issues as unique individuals, especially taking into account their personal concerns regarding vaccination. Due to time constricts on appointments and increased amounts of vaccine-hesitant clients, the capacity and confidence of health care providers are on ordeal. Health care providers need tools and training to face and answer the patients’ questions and concerns and thus, alleviate fears and remove mistrust regarding the vaccination. (Paterson et al. 2016; Di Pietro et al. 2017.) Also, general awareness about vaccinations as well as reasons behind vaccine hesitancy need to be raised.
Apichaya Korkawin and Ella Vehmas are graduating nursing students from LAB University of Applied Sciences. They have written the bachelor’s thesis Vaccination: Beliefs and Cultural Aspects.
Sini Hämäläinen works as a Senior Lecturer in LAB University of Applied Sciences.
References
Di Pietro, M., Poscia, A., Teleman, A., Maged, D. & Ricciardi, W. 2017. Vaccine hesitancy: parental, professional and public responsibility. Ann Ist Super Sanità. Vol 745.,11+ */3, No. 2. [Cited 28 Mar 2021]. Available at: https://www.iss.it/documents/20126/45616/ANN_17_02_13.pdf
Dube, E., Laberge, C., Guay, M., Bramadat, P., Roy, R. & Bettinger, J. 2013. Vaccine hesitancy. Landes Bioscience. [Cited 29 Jul 2020]. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3906279/
Korkawin, A. & Vehmas, E. [A3] 2021. Vaccination: beliefs and cultural aspects. Bachelor’s thesis. LAB University of Applied Sciences. [Cited 11.10.2021]. Available at: https://urn.fi/URN:NBN:fi:amk-2021100318262
Olson, O., Berry, C. & Kumar, N. 2020. Addressing Parental Vaccine Hesitancy towards Childhood Vaccines in the United States: A Systematic Literature Review of Communication Interventions and Strategies. Olson et al. [Cited 28 May 2020]. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7712553/
Paterson, P., Meurice, F., Stanberry, L., Glismann, S., Rosenthal, S. & Larson, H. 2016. Vaccine hesitancy and healthcare providers. Elsevier Ltd. Vol 24, No. 52. [Cited 26 Mar 2021]. Available at: https://www.sciencedirect.com/science/article/pii/S0264410X1630977X?via%3Dihub
Poland, G., Jacobson, R. & Ovsyannikova, I. 2009. Trends affecting the future of vaccine development and delivery: The role of demographics, regulatory science, the anti-vaccine movement, and vaccinomics. PMC. [Cited 3 May 2021]. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2693340/
Succi, R. 2018. Vaccine refusal – what we need to know. Jornal de Pediatria. Vol 94, No. 6. [Cited 29 Jul 2020]. Available at: https://www.sciencedirect.com/science/article/pii/S0021755717310045?via%3Dihub
WHO 2019. Ten threats to global health in 2019. [Cited 29 Jul 2020]. Available at: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019
Images
Image 1. huntlh. 2016. Influenssa, rokote, neula. Pixabay. [Cited 9 Oct 2021]. Available at: https://pixabay.com/fi/photos/influenssa-rokote-neula-oho-1719334/
Image 2. Sanofi Pasteur. 2021. Creative Commons Search. [Cited 9 Oct 2021]. Available at: https://search.creativecommons.org/photos/2f73abe1-cdd8-4678-95aa-f10adc019126




